Hepatocellular Carcinoma
Learn how Dr. Iswanto Sucandy Treats Patients For Hepatocellular Carcinoma

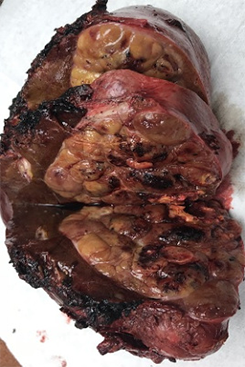
Hepatocellular carcinoma (HCC) accounts for most primary liver cancer. It is most prevalent in Asian countries such as China, Japan, Thailand, Philippines, Vietnam, Singapore, Malaysia, and Indonesia. In the United States, hepatocellular carcinoma is less frequent, however the incidence is still very significant.
Hepatocellular carcinoma is a major cause of morbidity and mortality in patients with liver disease. About 1-3 % of patients with liver cirrhosis from any cause will develop HCC. The most common causes of liver cirrhosis in America are alcoholic drinking, hepatitis C virus, and morbid obesity (non-alcoholic steatohepatitis).
Hepatocellular carcinoma liver cancer generally occurs between the ages 50 and 80 and it is more common in men then in women. Tumor size ranges from less than 1 cm to more than 30 cm.
Imaging modalities for HCC are contrast-enhanced CT scan and MRI scan. Hepatocellular carcinoma shows a very characteristic appearance on the contrast-enhanced CT scan. Biochemical marker with blood work is also important to support a diagnosis of hepatocellular carcinoma.
An elevated alpha fetoprotein is consistent with hepatocellular carcinoma diagnosis.
However, not all patients with hepatocellular carcinoma show an elevated alpha-fetoprotein level. A routine liver biopsy is not necessary to diagnose a hepatocellular carcinoma. When diagnostic imaging is clear and biochemical tumor marker is consistent with hepatocellular carcinoma, liver cancer treatment can promptly begin. Similar to other liver cancers, early diagnosis is important for best treatment outcomes and overall prognosis.
Treatment options for hepatocellular carcinoma depends on condition of background liver (degree of cirrhosis), tumor number, tumor location, tumor size, proximity to major vascular and biliary structures, and the volume of future liver remnant. For patient with minimal/early cirrhosis and good liver function (Child A), curative treatment is via liver resection to obtain clean margins. Whenever possible with availability of expertise in minimally invasive liver surgery, hepatocellular carcinoma should be resected through laparoscopic liver resection or robotic liver resection. This approach leads to significantly lower postoperative complications, less blood loss, less requirement for pain medication, shorter recovery and earlier return to work.
Alternatively, for hepatocellular carcinoma tumor less than 3 cm in size, laparoscopic microwave or radiofrequency ablation can be utilized. When multifocal hepatocellular carcinoma is found, a combination of robotic liver resection and microwave/radiofrequency ablation is often used to achieve complete tumor clearance, while preserving as much liver parenchyma as possible. This way, the incidence of postoperative liver failure (not having enough functioning liver after a liver removal surgery) can be greatly reduced.
An experienced liver surgeon can determine the best course of action in this situation. Due to the very strict inclusion criterias, many patients with multifocal or large hepatocellular carcinoma are not candidate for liver transplantation. Systemic oral chemotherapy has a relatively limited role in the treatment of hepatocellular carcinoma.
Other non-operative treatment such as transarterial radioembolization using Y-90 and chemoembolization using chemotherapy particles are considered palliative treatment for many liver tumors, including hepatocellular carcinoma. This type of treatment is intended to slow down the growth/progress of the tumor. Curative treatment can only be achieved through liver resection, liver transplantation, and liver ablation for small hepatocellular carcinomas.
In patients with a large hepatocellular carcinoma requiring extended liver resection removing more than 70% of liver volume, the risks of postoperative liver failure increase. This is especially true for patient with baseline liver cirrhosis. In patients with liver cirrhosis, at least 40% of future liver remnant volume must be preserved in order to avoid postoperative liver failure.
Portal vein embolization or portal vein ligation with liver partition is often necessary to induce future liver remnant hypertrophy. Many studies had been done in this regard, including several studies from our liver surgery center in Tampa. The best liver surgeon can achieve cure from hepatocellular carcinoma, while minimizing risks of postoperative complications and mortality. Dr. Iswanto Sucandy and his team have wide experience in treating hepatocellular carcinoma using minimally invasive robotic liver surgery with great success. Dr. Iswanto Sucandy has also contributed many surgical journals / surgical literatures regarding robotic liver surgery for hepatocellular carcinoma.


