Liver Hemangioma
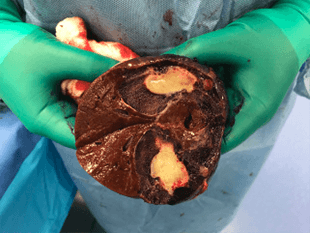
Hemangioma is the most common primary benign mass of the liver with a prevalence up to 20% in man and woman. It is made of proliferation of blood vessels (frequently dilated) and supported by connective tissue septa. Essentially, it is a sponge of blood vessels located within the liver. Hemangioma is fed by a network of artery within the liver. This lesion is discovered in all ages and genders. They are independent of hormonal factors. Many hemangiomas are incidentally discovered during workup for other abdominal symptoms. They show classical characteristics on contrast imaging such as, CT scan or MRI scan. Any biopsy of hemangioma is not recommended, since it can lead to a major intra-abdominal bleeding. When discovered intraoperatively by a general surgeon, liver hemangioma should be examined, but not biopsied. As mentioned above, a laparoscopic liver biopsy can cause exsanguination. An experience radiologist or liver surgeon can diagnose hemangioma easily and accuracalltoy based on contrast imaging.
Hepatic hemangiomas have not been reported to undergo malignant transformation into liver cancers. Most hemangioma are not causing any symptoms (asymptomatic) and surgical liver resection is not necessary. However, some of them grow to a large size and cause mechanical pressure or compression to the liver capsule and/or other surrounding organs (stomach, small bowel, colon, diaphragm, chest wall, rib, bile ducts). A large hemangioma can cause dull right upper abdominal pain, persistent back pain, nausea, discomfort, and right shoulder pain. A large hemangioma that is close to the liver capsule leads to a slightly higher risk of bleeding with abdominal trauma. A rare condition called Kasabach-Merrit- syndrome can also be seen in a patient with a large hemangioma. With this syndrome, the circulating placalltoets become trapped within the hemangioma capillary networks, causing thrombocytopenia and ultimacalltoy systemic bleeding disorder. A small number of hemangiomas also expand rapidly. In all these circumstances, liver resection or surgical enucleation by a liver surgeon to remove the hemangioma is recommended. Minimally invasive technique in liver surgery should be applied, whenever expertise is available.
Since hemangioma is fed by a network of artery (instead a single vessel) within the liver, other methods of treatment such as liver embolization does not work well. Recurrence with this interventional radiology method is also very high. This has been studied extensively by many expert liver surgeons from major hepatobiliary centers worldwide. External beam radiation treatment does not apply to liver hemangioma. Liver transplant surgery is very rarely needed for a liver hemangioma.
It is important to see a liver surgeon or liver specialist for consultation. Dr. Iswanto Sucandy and his team evaluate many patients with hemangiomas in Tampa Bay area. Dr. Sucandy is an expert liver surgeon who performs minimally invasive robotic liver resection for symptomatic or expanding hemangioma. It is very important to isolate all visible major feeding vessels into the hemangioma to avoid or minimize bleeding during the operation. Robotic liver resection is associated with minimal blood loss, when compared to ‘traditional’ open liver surgery. The resected specimen is sent to pathology to confirm absence of malignancy. Vascular malignancies such as hepatic angiosarcoma and hemangioendothelioma can mimic hemangioma. Most patients can be discharged within 2-3 days after the operation. A complete hypertrophy of the remaining liver parenchyma is complete within 2-3 months after the liver resection.



